Matrix-Based Hydrogels in Biomedical Applications: Design, Functionality, and Translational Insights
- Centre for Advanced Biotherapeutics and Regenerative Medicine, Faculty of Research, Chettinad Hospital and Research Institute, Chettinad Academy of Research and Education, Kelambakkam, India
- Centre for Herbal Pharmacology and Environmental Sustainability, Chettinad Hospital and Research Institute, Chettinad Academy of Research and Education, Kelambakkam, India
- Department of Natural and Applied Sciences, Nexus Institute of Research and Innovation (NIRI), Lalitpur, Nepal
Abstract
Hydrogels, defined as three-dimensional hydrophilic polymeric networks, have emerged as indispensable materials in drug delivery systems owing to their ability to encapsulate and release therapeutic agents in a controlled manner. Their structural characteristics closely mimic those of biological tissues, thereby enhancing biocompatibility and minimizing adverse systemic effects. Hydrogels can be engineered to respond to diverse physiological stimuli, such as pH and temperature, consequently facilitating the targeted release of drugs tailored to specific pathologies. Various crosslinking techniques, including physical and chemical methods, influence the mechanical stability and responsiveness of these materials, enabling advancements in applications ranging from tissue engineering to minimally invasive surgeries. Recent innovations include hybrid synthesis techniques that combine distinct crosslinking methods to augment the functional performance and customization of hydrogels. Furthermore, integrating biosensors and computational design methods into hydrogel frameworks holds promise for the development of autonomous systems capable of real-time therapeutic adjustments. In this review, we focus on the latest advancements in hydrogel design, with an emphasis on crosslinking strategies, stimulus-responsive mechanisms, and their integration into emerging biomedical applications. By synthesizing current research, we highlight the transformative potential of hydrogels in personalized medicine and their roles in addressing diverse clinical challenges.
Introduction
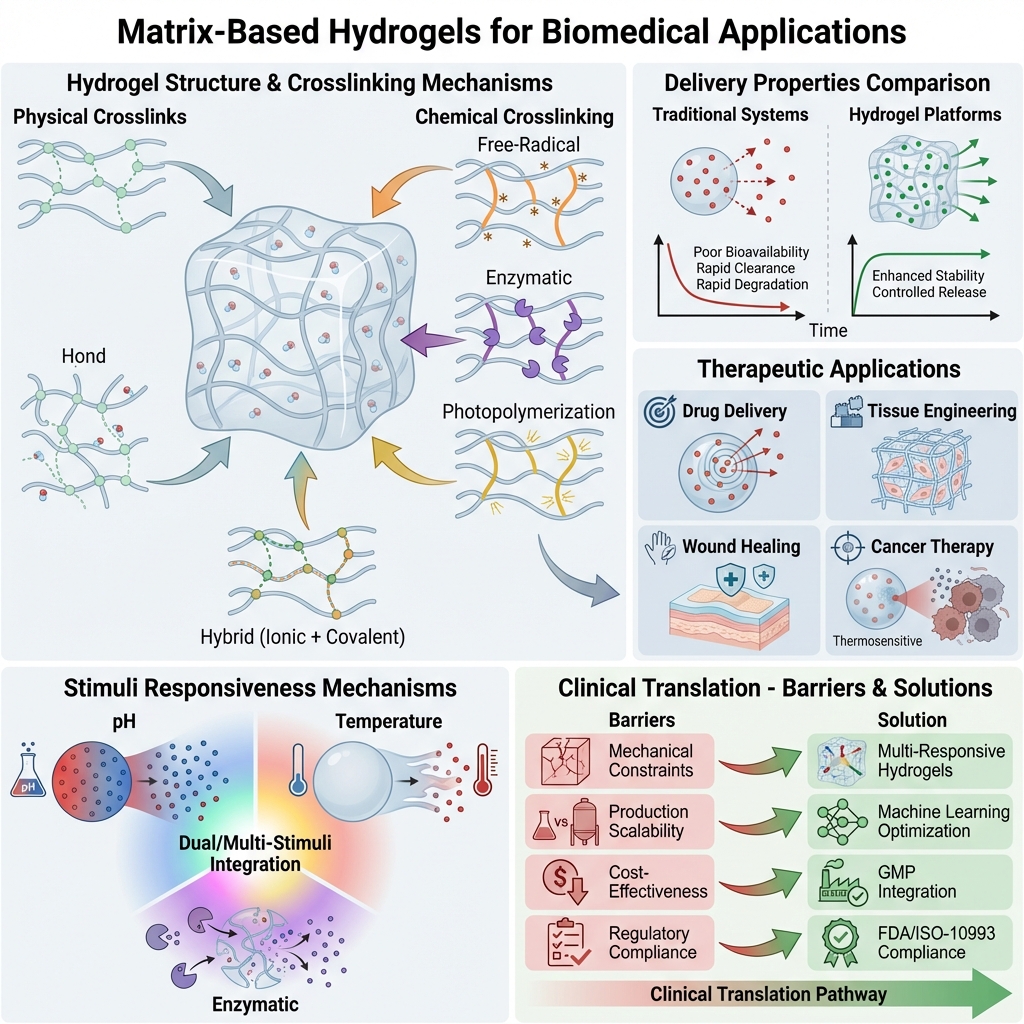
Hydrogels possess unique structural characteristics that enable them to closely mimic biological tissues, rendering them highly biocompatible and suitable for a myriad of biomedical applications 1. These matrices can encapsulate therapeutic agents and release them in a controlled and sustained manner, thereby addressing various therapeutic needs across disease contexts owing to their ability to retain water while maintaining structural integrity 2. Hydrogels play a pivotal role in modern drug delivery by facilitating targeted delivery and minimizing systemic side effects 3. The ability to incorporate responsive elements within hydrogels, such as pH, temperature, or enzyme sensitivity, further enhances their relevance in precision medicine, where treatments can be tailored to an individual’s unique biological environment (Figure 1). Overall, the flexibility, biocompatibility, and precision with which hydrogels control drug release make them indispensable for advancing therapeutic delivery.
Matrix-based hydrogels have been designed to address several critical challenges that have traditionally hindered effective drug delivery, including stability, bioavailability, and controlled release. Conventional drug delivery methods often suffer from poor bioavailability due to rapid drug clearance or degradation within the body. However, matrix-based hydrogels offer enhanced stability, creating a protective barrier around the encapsulated drug that prevents premature degradation and prolongs its therapeutic effects 4,5. In addition, matrix-based hydrogels provide a high degree of control over drug release profiles. By modifying the crosslinking density and molecular composition of the hydrogel matrix, researchers can design systems that release drugs over an extended period or in response to specific biological triggers. Furthermore, the development of matrix-based hydrogels aligns with the principles of personalized medicine, in which treatment regimens are tailored to individual patient profiles. For instance, pH-sensitive hydrogels with crosslinked networks can release drugs in response to the acidic environment of tumor tissues, thereby maximizing drug delivery efficacy while reducing off-target effects 6,7. Thus, matrix-based hydrogels can significantly improve the precision and efficacy of drug therapies, particularly in the treatment of chronic diseases such as cancer, diabetes, and cardiovascular conditions, where conventional drug delivery methods are often inadequate.
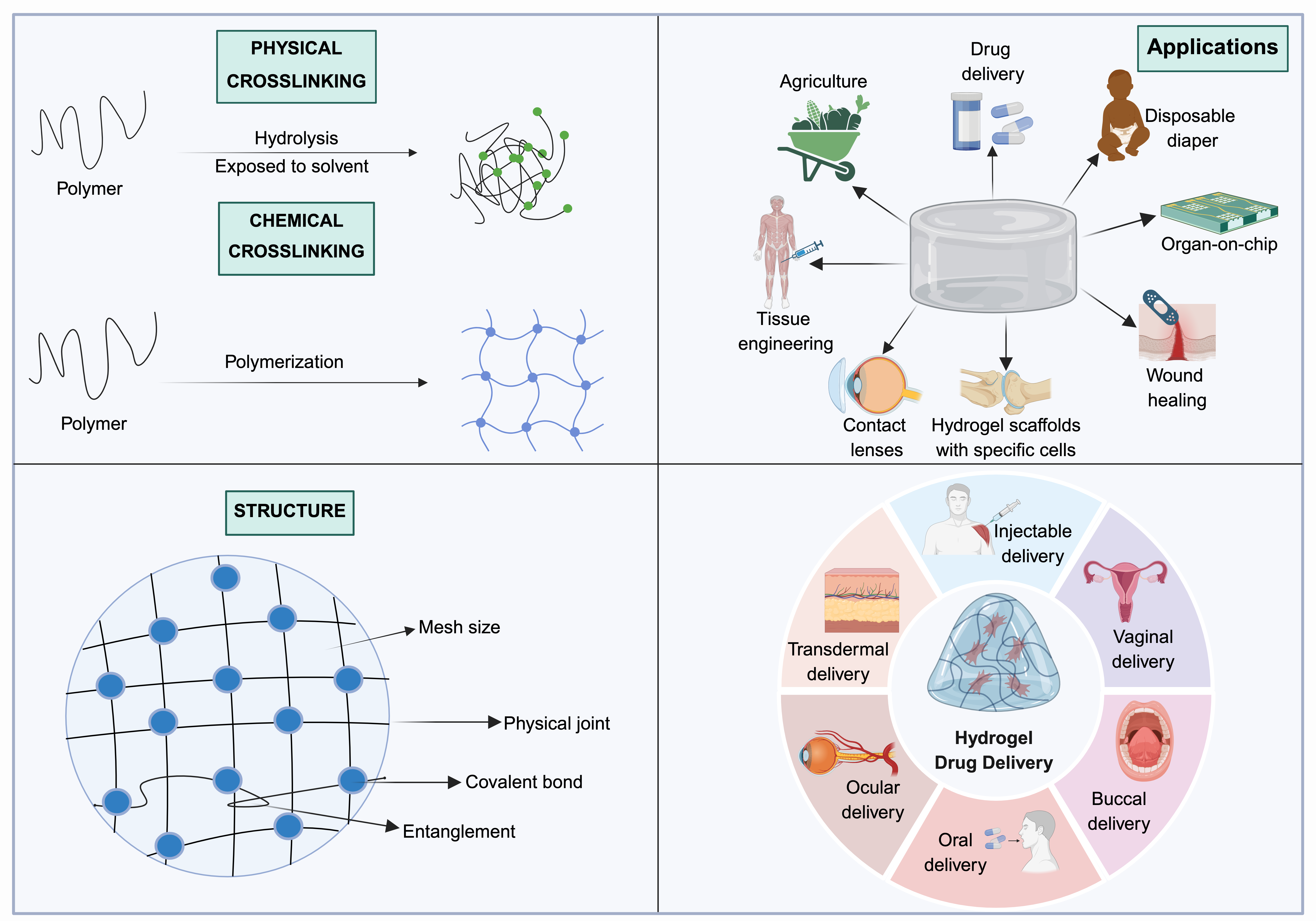
In the top-left corner, physical and chemical crosslinking are illustrated; the bottom-left corner displays the structure of the hydrogel as defined by mesh size, covalent bonds, and physical entanglements; the top-right corner presents applications of the hydrogel, including drug delivery, tissue engineering, agriculture, and consumer products; and the bottom-right corner depicts the hydrogel and its delivery routes.
Literature search strategy and selection criteria
In this narrative review, we systematically present matrix-based hydrogels and their biomedical applications. We conducted a comprehensive database search across ScienceDirect, PubMed, Web of Science (WOS), and Scopus using a strategy that combined keywords with Boolean operators: “Hydrogel,” “matrix-based hydrogel,” “Drug delivery,” and “Biomedical application” (Figure 2). All studies published between 2015 and 2025 were initially screened based on their titles and abstracts to eliminate duplicates and irrelevant literature. Full-text English articles were then assessed for eligibility. The inclusion criteria comprised original research, reviews, books, and clinical trials that focused on matrix-based hydrogel design, crosslinking, properties, and biomedical applications. Editorials, commentaries, and conference proceedings without primary data were excluded. Following screening, the studies deemed eligible for this review were included in the qualitative analysis. A narrative synthesis approach was employed due to the inherent variability in study design and reporting. Data were manually extracted using a standardized framework to document hydrogel composition, fabrication, crosslinking, functional features, and biomedical applications.
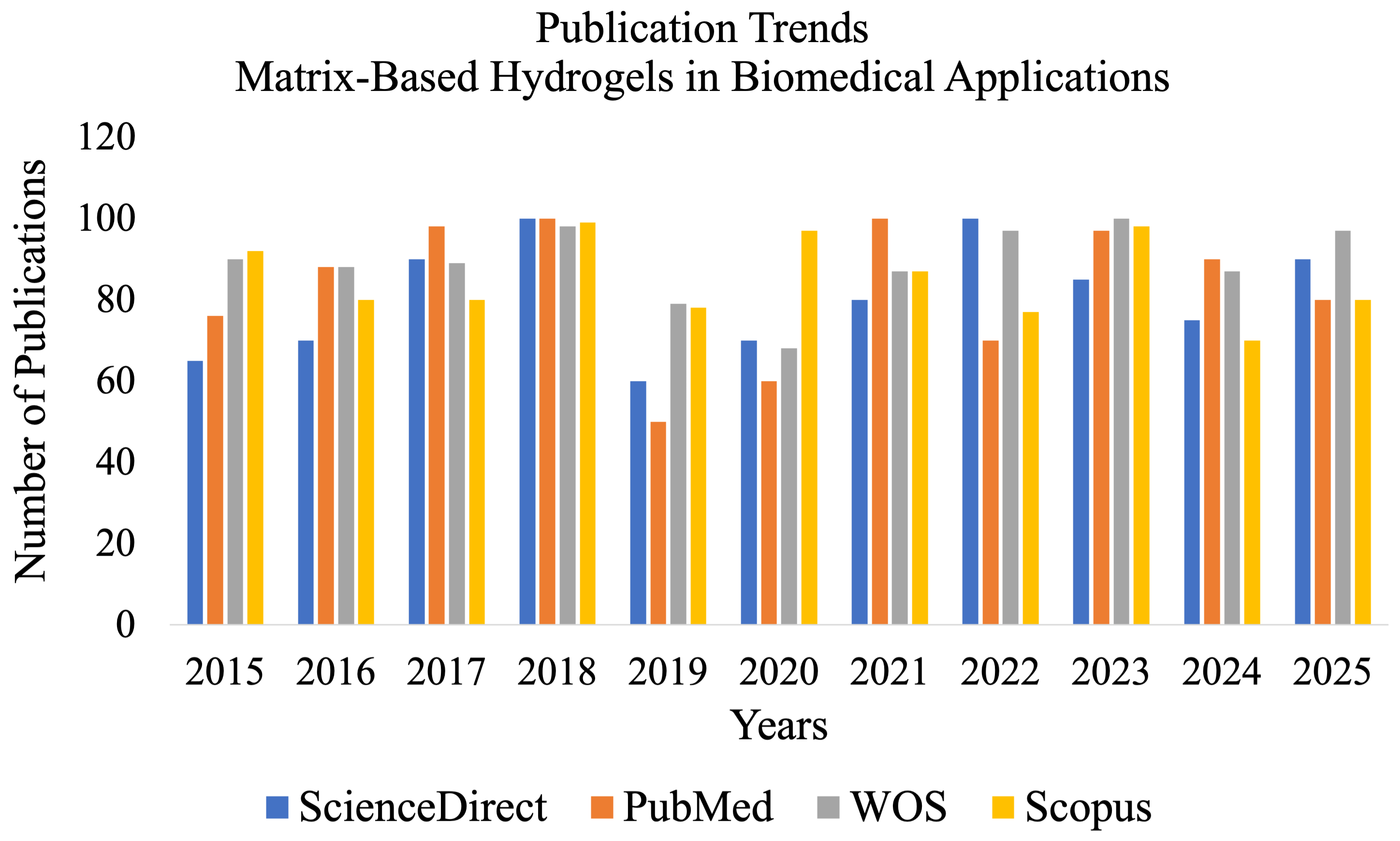
Annual publication trends in matrix-based hydrogel research for biomedical applications from 2015 to 2025 were compiled from ScienceDirect, PubMed, WOS, and Scopus. Publication counts reflect database-indexed records and research volumes, which may include duplicate entries. These data do not indicate study quality or include statistical comparisons or error bars. Trends over the years may have been affected by reporting and publication biases.
Materials Fundamentals of Matrix-Based Hydrogels
The performance of matrix-based hydrogels in biomedical systems fundamentally depends on their internal architecture, which is governed by both the synthesis route and crosslinking mechanism. This section integrates these two core design parameters into a unified framework, detailing how the polymer source, network-forming chemistry, and fabrication methods determine mechanical integrity, degradation, and therapeutic suitability. The translational implications of each approach are emphasized, bridging materials science with regulatory and clinical perspectives. The most commonly used methods for hydrogel preparation are tabulated in Table 1. Methods such as radiation crosslinking and free radical polymerization are preferred for large-scale production because of their efficiency and reliability. Simpler methods, such as physical crosslinking or freeze-thaw cycling, are cost-effective and commonly utilized for low-tech applications.
Common methods for preparing hydrogels primarily focus on commercially available options and their applications in various fields.
| S.N. | Preparation method | Process | Example | Key controllable parameters | Application | Reference |
|---|---|---|---|---|---|---|
| 1 | Physical crosslinking | |||||
| a. | Ionic gelation | Polymers with ionic groups interact with counter ions to form hydrogel. | Alginate with calcium ions forms a hydrogel matrix. | Ion concentration, polymer molecular weight, gelation time, ionic strength | Drug delivery systems, tissue engineering, and wound dressings. | |
| b. | Hydrogen bonding or hydrophobic interactions | Hydrogels form through secondary interactions, such as hydrogen bonding or hydrophobic interactions. | Gelatin or poly(vinyl alcohol) (PVA) hydrogel. | Polymer concentration, temperature, pH, solvent composition | Soft contact lenses and biomedical scaffolds. | |
| c. | Freeze-thaw cycling | Repeated freezing and thawing cycles create crystalline regions that act as physical crosslinks. | PVA hydrogels. | Number of freeze-thaw cycle, freezing temperature, thawing duration | Artificial cartilage, tissue engineering. | |
| 2 | Chemical crosslinking | |||||
| a. | Radiation-induced crosslinking | High-energy radiation induces free radical formation, leading to polymer crosslinking. | PVA or poly(ethylene glycol) (PEG) hydrogel. | Radiation dose, exposure time, polymer concentration | Wound dressings, drug delivery, and agriculture. | |
| b. | Chemical crosslinking | Chemical agents link the polymer chains. | Collagen or hyaluronic acid hydrogel. | Crosslinker type, crosslinker concentration, reaction time, pH | Drug delivery systems and tissue scaffolds. | |
| c. | Enzymatic crosslinking | Enzymes catalyze the covalent bond formation between polymers. | Fibrin-based hydrogels. | Enzyme concentration, reaction time, substrate availability | Wound healing and tissue regeneration. | |
| 3 | Polymerization methods | |||||
| a. | Free radical polymerization | Monomers are polymerized using initiators and crosslinkers. | Polyacrylamide hydrogel. | Initiator concentration, crosslinker ratio, polymerization time | Superabsorbent materials, biomedical devices. | |
| b. | Photopolymerization | UV or visible light initiates polymerization of photosensitive monomers, | PEG-diacrylate hydrogels. | Photo-initiator type, light wavelength, irradiation time | Dental materials, 3D-printed hydrogel. | |
| 4 | Self-assembly | Amphiphilic molecules and peptides spontaneously organize into gels in aqueous environments. | Peptide-based hydrogels. | Peptide sequence, concentration, ionic strength, and temperature. | Injectable hydrogels, tissue engineering, drug carriers. | |
| 5 | Interpenetrating polymer networks (INs) | IPNs combine two polymers, one of which is synthesized or cross-linked in the presence of the other. | Polyacrylamide-alginate hydrogels. | Relative polymer ratios, crosslinking order, and network density. | Biomaterials, sensors, and controlled drug release. | |
| 6 | Emulsion polymerization | Monomers are dispersed in an oil phase and polymerized to form hydrogel microspheres or particles. | Polyacrylate super-absorbents. | Droplet size, surfactant concentration, and polymerization conditions. | Agriculture, hygiene products, and pharmaceuticals. | |
| 7 | Microwave-assisted synthesis | Microwave irradiation accelerates crosslinking or polymerization. | Various synthetic hydrogels | Microwave power, exposure time, and solvent system. | Industrial hydrogel production is driven by rapid and energy-efficient synthesis. | |
| 8 | Template-assisted synthesis | Hydrogels are formed within molds or templates to achieve specific shapes or structures. | Hydrogel microparticles or nanogels. | Template geometry, polymer concentration, and curing conditions. | Drug carriers and biosensors. | |
Crosslinking Mechanisms and Structural Control
Crosslinking is central to hydrogel formation, enabling the fabrication of three-dimensional networks with tunable porosity, mechanical stability, and biofunctionality. Traditionally, crosslinking methods are categorized as physical or chemical, each offering distinct structural and translational characteristics 33. Physical crosslinking relies on non-covalent interactions, such as hydrogen bonding, hydrophobic interactions, and ionic interactions with divalent cations ($Ca^{2+}$), yielding reversible, biocompatible gels. Poly(N-isopropylacrylamide) (PNIPAAm)-based thermoresponsive systems that undergo sol–gel transitions near physiological temperatures exemplify their utility in minimally invasive, injectable platforms 34. Their chemical simplicity and cytocompatibility make them attractive candidates for wound dressings and cell encapsulation. However, their mechanical frailty and batch-to-batch variability hinder their approval for load-bearing applications 35.
In contrast, chemical crosslinking produces covalently stabilized networks with superior mechanical and chemical stability. Common strategies include free-radical polymerization, enzymatic crosslinking, and photopolymerization. For example, genipin and glutaraldehyde confer long-term resilience but pose cytotoxicity risks if residues remain, whereas photo-initiator-based PEG systems allow spatiotemporal control of patient-specific scaffold fabrication 36. Enzyme-mediated methods using horseradish peroxidase or transglutaminase mitigate toxicity concerns and preserve bioactivity; however, industrial scale-up remains technically demanding.
Synthesis and Fabrication Techniques
Hybrid crosslinking approaches that combine ionic and covalent interactions are gaining attention for balancing injectability and durability. Ionically stabilized alginate matrices reinforced with covalent bonds demonstrate superior toughness while retaining biocompatibility 37. These hybrid gels align with the Food and Drug Administration (FDA) combination product standards but require rigorous reproducibility to meet the Good Manufacturing Practice (GMP) and International Organization for Standardization (ISO-10993) criteria 38. Ultimately, the crosslinking strategy dictates not only the drug release kinetics and degradation behavior but also the regulatory classification and clinical safety assessment. The reported fabrication parameters for chemically crosslinked hydrogels vary significantly across studies; for example, photopolymerized PEG-based systems typically use low millimolar photoinitiator concentrations and irradiation times of seconds to minutes, depending on the gel thickness and application.
Hydrogel synthesis determines the microarchitecture, porosity, and encapsulation efficiency, which directly impact therapeutic delivery and tissue interaction. The choice of fabrication method balances the structural precision, scalability, and regulatory compliance. Physical and chemical preparation methods include ionic gelation, freeze–thaw cycling, radiation crosslinking and enzymatic processes. Simpler physical routes are cost-effective and ideal for low-tech biomedical applications, whereas chemical and radiation-induced methods are well-suited for industrial-scale production because of their reproducibility. Bulk polymerization produces dense, mechanically robust networks suitable for implantable depots; however, residual initiators can impair biocompatibility. Solution polymerization yields hydrated, uniform gels ideal for encapsulating labile biomolecules, whereas emulsion polymerization enables the controlled formation of micro- and nanogels for targeted delivery. Graft copolymerization introduces responsive functional groups for “smart” hydrogels that adapt to local pH, temperature, or enzymatic cues, which is an essential feature for precision drug release in oncology 39. Emerging synthesis platforms, such as 3D-bioprinting and microwave-assisted polymerization, bridge the gap between laboratory customization and scalable manufacturing 30. However, clinical translation requires validation of batch uniformity, sterilization compatibility, and the safety of degradation byproducts, as emphasized by the FDA and the European Medicines Agency (EMA).
Translational Implications and Regulatory Context
The material foundation of hydrogels has direct regulatory implications. The FDA’s 21 CFR Part 820 and ISO-10993 standards emphasize the need for reproducibility, biocompatibility, and defined degradation profiles 40. Crosslinking chemistry influences the categorization of hydrogels as medical devices, drug delivery systems, or combination products 41. For instance, chemically crosslinked PEG-based scaffolds must demonstrate consistent long-term mechanical and chemical stability, whereas physically crosslinked hydrogels require extensive leaching and degradation testing because of their labile nature. Integrating GMP-compliant synthesis early in development accelerates approvals and ensures scalability 42. Moreover, hybrid and stimuli-responsive gels are increasingly being evaluated under adaptive regulatory frameworks that encourage the modular testing of multifunctional materials.
Key Takeaways of Materials Fundamentals
Hydrogel properties arise from the interplay between crosslinking chemistry and fabrication techniques, which determine biocompatibility, stability, and release behavior. Hybrid crosslinking and stimuli-responsive architectures represent the next generation of clinically adaptable hydrogels 43. Regulatory success depends on reproducibility, sterilization stability, and ISO-10993–compliant evaluation of degradation and cytotoxicity. The merging of synthesis and crosslinking perspectives provides a unified material foundation for understanding hydrogel performance across biomedical applications.
Recent Advances in Hydrogel Applications
Hydrogels are increasingly recognized for their versatility across a wide range of biomedical applications, largely due to their high water content, biocompatibility, and adjustable physical and chemical properties. Recent advancements in hydrogel design have facilitated significant progress in various medical fields, including targeted drug delivery, tissue engineering, wound healing, cancer treatment, and biosensing. This section examines these developments, emphasizing how novel materials, synthesis techniques, and functionalization strategies have broadened the potential of hydrogels for medical and therapeutic applications (Figure 3). Hydrogels have undergone substantial evolution in recent years, with enhancements in their design, functionality, and applications (Table 2).
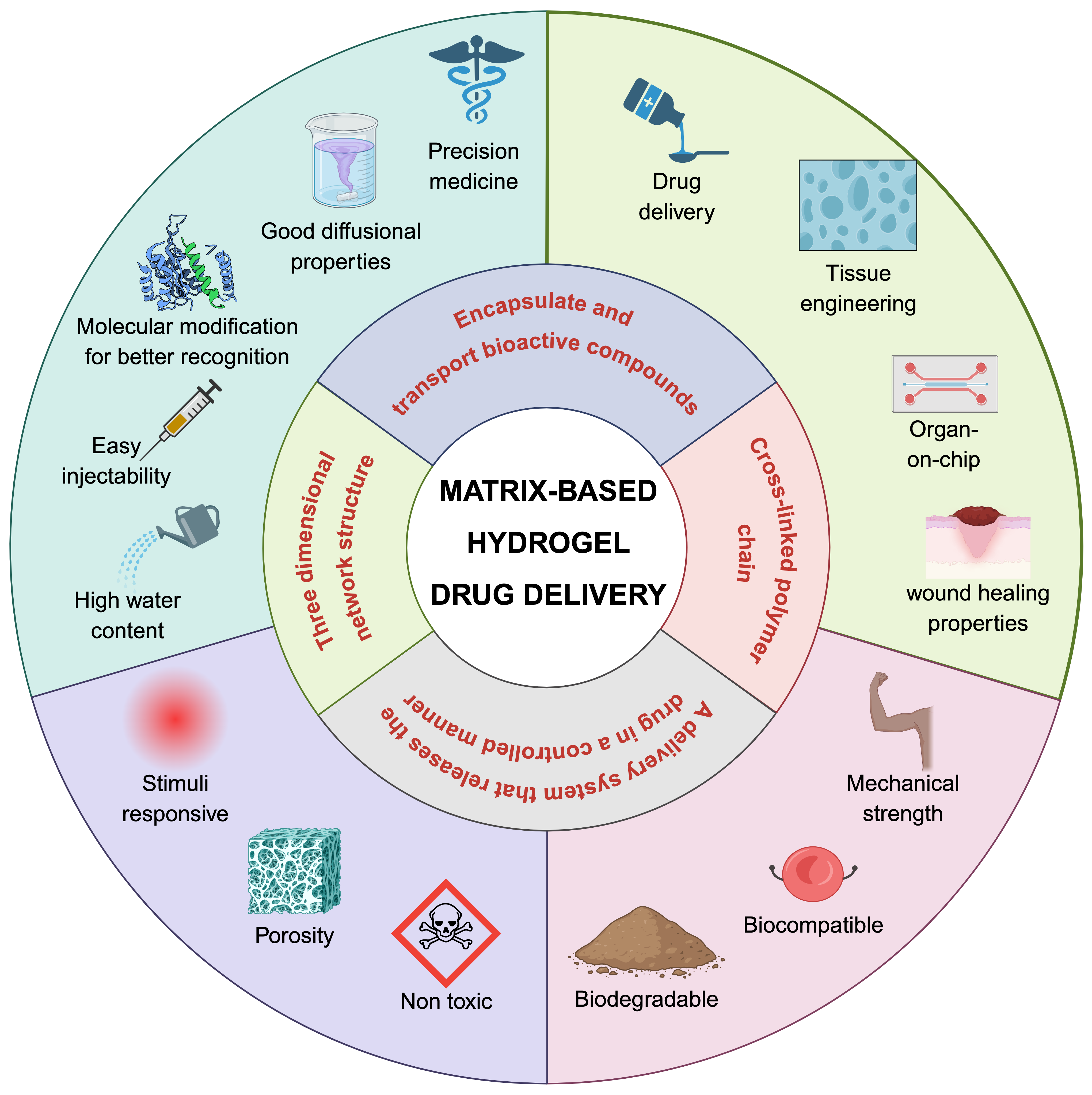
Multifaceted capabilities of matrix-based hydrogel drug carriers. These systems are designed to encapsulate and deliver bioactive compounds, enabling controlled drug release for applications such as precision medicine, targeted drug delivery, tissue engineering and wound healing. The versatility of these hydrogels stems from their tunable properties, including good diffusional characteristics, potential for molecular-level modifications that enhance recognition, ease of injection, high water content, responsiveness to external stimuli, controlled porosity, non-toxicity, biodegradability, robust mechanical strength, and inherent biocompatibility. This combination of features positions matrix-based hydrogels as promising tools for developing sophisticated therapeutic interventions.
Overview of recent biomedical advances in hydrogel applications.
| S.N. | Applications | Advances | Examples | References |
|---|---|---|---|---|
| Biomedical applications | ||||
| 1 | Drug delivery systems |
Stimuli-responsive hydrogels: Hydrogels that respond to pH, temperature, enzymes, or light for controlled and targeted drug release. Self-healing hydrogels: Enhancing reusability and adaptability for long-term drug delivery | Delivery of chemotherapeutics, antibiotics, and biologics, including monoclonal antibodies and mRNA. | |
| 2 | Tissue engineering and regenerative medicine |
3D-Printed hydrogels: Customized tissue scaffolds using bioinks derived from hydrogels. Dynamic hydrogels: Hydrogels that can adapt to changing mechanical environments and mimic native tissues. Hybrid hydrogel: Combination of natural and synthetic polymers for enhanced biocompatibility and mechanic strength. | Bone, cartilage, skin, and neural tissue engineering. | |
| 3 | Wound healing and skin regeneration |
Antibacterial hydrogels: Incorporation of nanoparticles or antimicrobial peptides. Oxygen-releasing hydrogels promote faster healing in hypoxic wound environments. Thermosensitive hydrogels: Form at body temperature to conform to irregular wound shapes. | Diabetic ulcers, burns, and chronic wounds. | |
| 4 | Soft robotics and wearable devices |
Conductive hydrogels: Hydrogels integrated with ionic liquids or conductive polymers for sensing or actuation. Stretchable Hydrogels: Hydrogels with exceptional elasticity for wearable sensors. | Bioelectronics, artificial muscles, and real-time health monitoring. | |
| 5 | Cancer research and therapy |
Hydrogel-based immunotherapy: Hydrogels serve as platforms for delivering immune-stimulating agents or vaccines for cancer treatment. 3D-Tumor Models: Hydrogels mimic tumor microenvironments for drug testing and cancer research. Nanoparticle-loaded hydrogels enable the localized delivery of chemotherapy or gene-editing tools, such as CRISPR/Cas9. | Personalized cancer treatment and preclinical testing. | |
| Progressive advancement in applications | ||||
| 1 | Advanced diagnostics and biosensing |
Hydrogel sensors: Embedded with fluorescence or electrochemical elements for biomolecule detection. Self-adhesive hydrogels: Hydrogels that adhere to tissues for in situ diagnostics. | Point-of-care testing, wearable diagnostics, and real-time monitoring of physiological conditions. | |
| 2 | Advances in hydrogel design |
Hybrid hydrogels: Combining natural and synthetic polymers to improve properties such as biocompatibility, mechanical strength, and stimuli responsiveness. Multi-stimuli-responsive hydrogels: hydrogels that respond to two or more stimuli for complex applications. Nanocomposite hydrogels: Integration of nanoparticles or nanostructures for enhanced functionality. | Tumor microenvironment-sensitive hydrogels for cancer drug delivery and wound healing. | |
Targeted Drug Delivery
Stimuli-responsive hydrogels that react to pH, temperature, or enzymatic cues have shown promise for site-specific drug release, minimizing systemic toxicity in diseases such as cancer 62. Recent innovations have introduced dual- and multi-stimuli-responsive hydrogels that respond to combinations of stimuli, providing greater control over the drug release. Beyond cataloguing responsive modalities, a pattern emerges when comparing high-performing systems: performance correlates with the orthogonality of the stimuli and polymer network mechanisms. For example, dual-responsive hydrogels that combine pH-driven ionic swelling with thermoresponsive phase transitions (e.g., ionic polysaccharides crosslinked into PNIPAAm networks) typically exhibit sharper and more reproducible release profiles than systems that attempt to couple two mechanisms that operate through the same physical pathway (e.g., two diffusion-limited mechanisms). This suggests that synergy, rather than redundancy, between stimuli mechanisms underlies the superior control of release 63.
The divergence between studies is often explained by differences in crosslink density, network reversibility, and drug–matrix interactions. Systems with reversible, dynamic crosslinks (e.g., ionic or supramolecular bonds) recover their barrier function after stimulus removal, providing pulseable release, whereas permanently crosslinked networks tend to exhibit unidirectional release driven by degradation 64. Similarly, hydrophobic drug payloads interact strongly with hydrophobic domains in the matrix, slowing their release compared with hydrophilic drugs, where diffusion dominates. These mechanistic differences explain why nominally similar dual-stimulus hydrogels can produce markedly different pharmacokinetics in vivo. Finally, many promising preclinical studies lack robust pharmacokinetic and toxicological validation. Key translational barriers are batch-to-batch reproducibility of stimulus responsiveness and long-term biocompatibility of degradation products; addressing these requires standardized stimulus-challenge assays and long-term in vivo monitoring before clinical translation.
Tissue Engineering and Regenerative Medicine
Hydrogels and electrospun nanofibers are foundational biomimetic scaffolds in tissue engineering and regenerative medicine because they closely mimic the natural extracellular matrix (ECM), thereby supporting cell function and tissue formation 65,66. A central analytical consideration in selecting a hydrogel (natural or synthetic) involves a fundamental trade-off between intrinsic bioactivity and mechanical tunability 67. Natural hydrogels (collagen, hyaluronic acid, and alginate) provide integrin-binding sites and native signaling that promote cell adhesion and differentiation; however, their mechanical weakness and batch variability limit their use in load-bearing applications 68. Synthetic polymers (PEG, PVA, PNIPAAm) provide reproducible mechanical properties and tunable degradation but require biofunctionalization (e.g., arginylglycylaspartic acid (RGD) peptides, growth factor tethering) to recapitulate cell–matrix interactions. Mechanistically, successful scaffolds reconcile matrix mechanics (stiffness and viscoelasticity) with biochemical presentation (ligand density and mobility) 69. For example, PEG hydrogels functionalized with controlled RGD density and nanoparticle or fiber reinforcement can match the osteogenic cues of the natural ECM while retaining the mechanical strength required for bone repair 70. Divergent clinical outcomes across studies often stem from inconsistent reporting of crosslinking chemistry and ligand presentation; small changes in functionalization density or crosslinker type can shift cell fate decisions (e.g., osteogenesis vs. adipogenesis). Standardized mechanical and biochemical characterizations (e.g., stress relaxation and ligand quantification) will improve comparability and translation 71. The development of self-healing hydrogels and composites that combine hydrogel matrices with reinforcing fibers and nanoparticles is a promising area of research. However, it requires rigorous testing for wear, fatigue, and host responses under physiological loads before regulatory approval 72,73. Natural and synthetic matrix-based hydrogels exhibit distinct strengths and limitations depending on the clinical indications (Table 3).
Focused comparisons of natural and synthetic matrix-based hydrogels in clinically relevant applications.
| Clinical Indication | Natural Hydrogels (Collagen, HA, Alginate) | Synthetic Hydrogels (PEG, PVA, PNIPAAm) | Reference |
|---|---|---|---|
| Cartilage Repair | Promote chondrocyte adhesion and ECM production; high bioactivity; poor load-bearing and fast degradation | High mechanical tunability; customizable degradation; require biofunctionalization for cell adhesion | |
| Dermal (Wound Healing) | Collagen/ gelatin provide intrinsic bioactivity, hemeostasis, and cell infiltration; limited control over degradation | PEG/PVA systems offer controlled drug release, stability, and tunable porosity; lower intrinsic bioactivity | |
| Ocular Applications | HA/alginate improve lubrication, muco-adhesion, and drug retention; rapid clearance limits sustained delivery | PNIPAAm/PEG allow thermo-responsive gelation, sustained release, and reproducibility; may lack native cell signaling cues |
Wound Healing
The high water content and permeability of hydrogels create ideal moist wound environments that accelerate healing 80. A comparative evaluation of antimicrobial strategies revealed a spectrum of trade-offs: inorganic agents (silver nanoparticles) exhibited broad-spectrum antimicrobial activity. They are effective against multidrug-resistant (MDR) organisms but may cause cytotoxicity and oxidative stress at higher doses 81. Biopolymeric antimicrobials (e.g., chitosan and antimicrobial peptides) often strike a better balance between antimicrobial potency and host cell compatibility but can be more sensitive to proteolytic degradation in wound exudates. Mechanistically, nanoparticle inclusion alters the local redox balance and can trigger inflammatory responses if not tightly controlled; therefore, optimizing the particle load, release kinetics, and surface chemistry is critical. Several studies have demonstrated improved healing rates in animal models. However, divergent clinical efficacy likely reflects differences in the wound environment (chronic vs. acute), hydrogel degradation behavior, and local immune milieu. Post-marketing surveillance focusing on the emergence of resistance, local tissue compatibility, and systemic absorption is essential for the safe translation of drugs 82.
Cancer Therapy
Hydrogels for cancer therapy function as local drug depots, enabling concentrated drug delivery and multimodal therapies (chemotherapy, immunotherapy, and photothermal therapy) 83. Comparative analyses have indicated that minimally invasive, injectable thermosensitive hydrogels exhibit reliable in situ gelation; however, they require precise control over gelation kinetics and in vivo mechanical stability to avoid premature leakage 84,85. Hybrid hydrogel–nanoparticle systems often outperform hydrogel-only systems for photothermal or immune-adjuvant applications because the nanoparticle can confine heat or modulate immune activation; however, nanoparticle size, shape, and surface chemistry strongly influence biodistribution and immunogenicity 86. For instance, well-dispersed gold nanorods yield homogeneous photothermal profiles and predictable heating, whereas aggregated or irregular nanoparticles cause hotspot formation and unpredictable tissue damage. Translationally, scaling production under GMP and demonstrating superiority over established delivery modalities in randomized controlled trials remain major hurdles.
Bio-sensing and Diagnostics
Hydrogels in biosensors act as matrices for immobilizing biomolecules while allowing analyte diffusion 87,88. Comparative strengths show that enzyme-based hydrogels excel in sensitivity but suffer from limited operational stability due to enzyme denaturation. conductive polymer–hydrogel composites offer improved durability and signal transduction but less biological specificity 89. The reproducibility of the signal response depends on uniform immobilization, hydrogel porosity, and fouling resistance. Integrating hydrogels into wearable or implantable sensors requires controlling hydration, mechanically matching the tissue, and developing robust calibration protocols, areas where the current literature diverges widely in methodology. Systematic benchmarking across physiological ranges and long-term patient data are required to transition from prototype to approved diagnostics 90,91.
Hydrogel-based scaffolds and organ-on-chip
Hydrogels, as scaffolds for organ-on-chip platforms, provide physiologically relevant microenvironments and reduce the need for animal testing 92. Organ-on-chip systems use hydrogels as scaffolding materials to mimic the ECM, thereby providing a biocompatible and tunable microenvironment for cellular growth and function (Figure 4). An analytical comparison of studies revealed a key design axis: mechanical fidelity and mass transport 93. Hydrogels that faithfully mimic tissue stiffness can impede perfusion and nutrient transport if their porosity is low. Conversely, highly permeable gels may fail to provide appropriate mechanical cues for cell polarization and migration. Additionally, dynamic or responsive hydrogels (e.g., with tunable crosslinking or embedded growth factors) better capture tissue remodeling but introduce complexity in terms of reproducibility and cross-platform validation. Regulatory frameworks lag behind these advances; the standardization of mechanical, biochemical, and microfluidic performance metrics is essential to enable clinical and industrial adoption 92. Despite remarkable advances, the clinical success of hydrogel-based technologies remains limited compared with their preclinical promise. Bridging this gap requires rigorous multi-omics validation, GMP-compliant manufacturing processes, long-term safety studies, and alignment with relevant regulatory standards. A stronger integration of clinical trial data with laboratory innovations is essential for hydrogels to evolve from research tools into mainstream therapeutic platforms.
Limitations of publication trends and temporal coverage
Although the growing number of hydrogel-related publications reflects continued academic and industrial interest, it is important to interpret these trends carefully. Bibliometric analyses based on indexed databases are affected by publication bias, including a tendency to report positive or successful results more often, underrepresent negative or inconclusive studies, and delay the publication of translational failures. Consequently, increasing publication numbers do not always correspond to equivalent progress in clinical readiness or regulatory approval. Additionally, although this review includes literature up to 2025, rapidly emerging fields such as AI-assisted hydrogel design, regulatory-guided manufacturing strategies, and organ-on-chip validation may not yet be fully captured in peer-reviewed sources. Regular updates through systematic review frameworks are essential to maintain an accurate and up-to-date assessment of progress in this area.
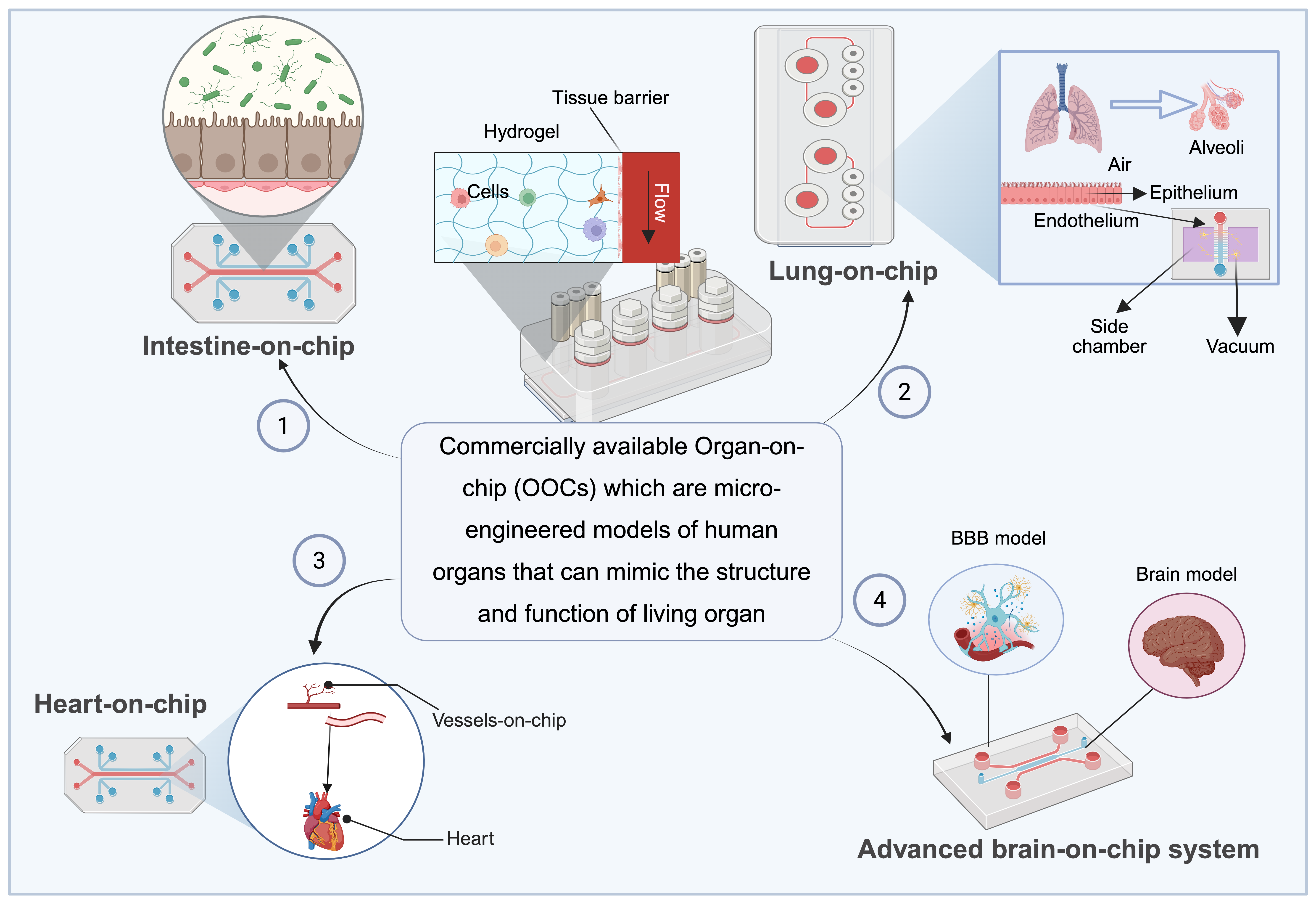
Overview of technological advancements in various commercially available organ-on-chip models. These are micro-engineered systems that mimic the structure and function of human organs. The models highlight several prominent applications, including the intestine, lung, heart, and advanced brain-on-a-chip models that utilize microfluidics and cell culture to simulate organ-level physiology
Ongoing Clinical Trials/ Translational Insights
Although matrix-based hydrogels have advanced rapidly in preclinical models, the clinical portfolio remains concentrated in a few application domains: wound management, soft-tissue augmentation, and localized drug depots, while definitive trials for more complex indications (e.g., load-bearing tissue regeneration and intratumoral drug release) are still emerging. Several ongoing clinical studies have demonstrated the translational breadth of matrix-based hydrogels in surgical reconstruction, wound care, orthopedics, and intervertebral disc repair (Figure 5). The role of a self-assembling RADA16 peptide hydrogel (PuraGel) is being assessed in endoscopic skull base surgery to expedite mucosal healing of nasoseptal flap donor sites and reduce sinonasal morbidity following cranial base procedures (interventional; recruiting). This trial evaluated wound healing and postoperative sinonasal outcomes, providing evidence for the regenerative applications of short-peptide hydrogels in soft tissues 94. A randomized study ( comparing an acellular dermal matrix (ADM) hydrogel with conventional alginate dressings is planned to determine whether the ADM hydrogel accelerates wound closure in chronic traumatic wounds and improves the local tissue quality. This study (sponsor: Isfahan University of Medical Sciences) will determine whether biologically derived hydrogel matrices can outperform standard care in chronic wound management and whether they meet clinical endpoints, such as wound area reduction at 12 weeks. In orthopedics (), a multicenter, randomized, controlled trial is comparing JointRep (a matrix scaffold/hydrogel adjunct) plus microfracture with microfracture alone for focal chondral defects, evaluating both functional and structural outcomes (e.g., patient-reported outcomes and imaging endpoints) 95. This study aimed to determine whether hydrogel-augmented cartilage repair confers durable functional benefits compared to established surgical techniques. Collectively, these trials highlight two important translational themes: (1) matrix-based hydrogels are being tested across diverse anatomic sites and indications, often with primary endpoints anchored to local tissue healing, pain relief, or functional restoration rather than long-term survival; and (2) early phase studies prioritize safety, biocompatibility, and surrogate efficacy measures—outcomes that must be bridged to larger randomized trials with clinically meaningful endpoints for definitive regulatory acceptance. To accelerate translation, future trials should harmonize biomaterial characterization (International Organization for Standardization, ISO-10993 testing, and GMP specifications), incorporate standardized clinical endpoints and imaging/biomarker panels to enable cross-study comparisons, and include longer follow-ups to capture durability and late adverse events.
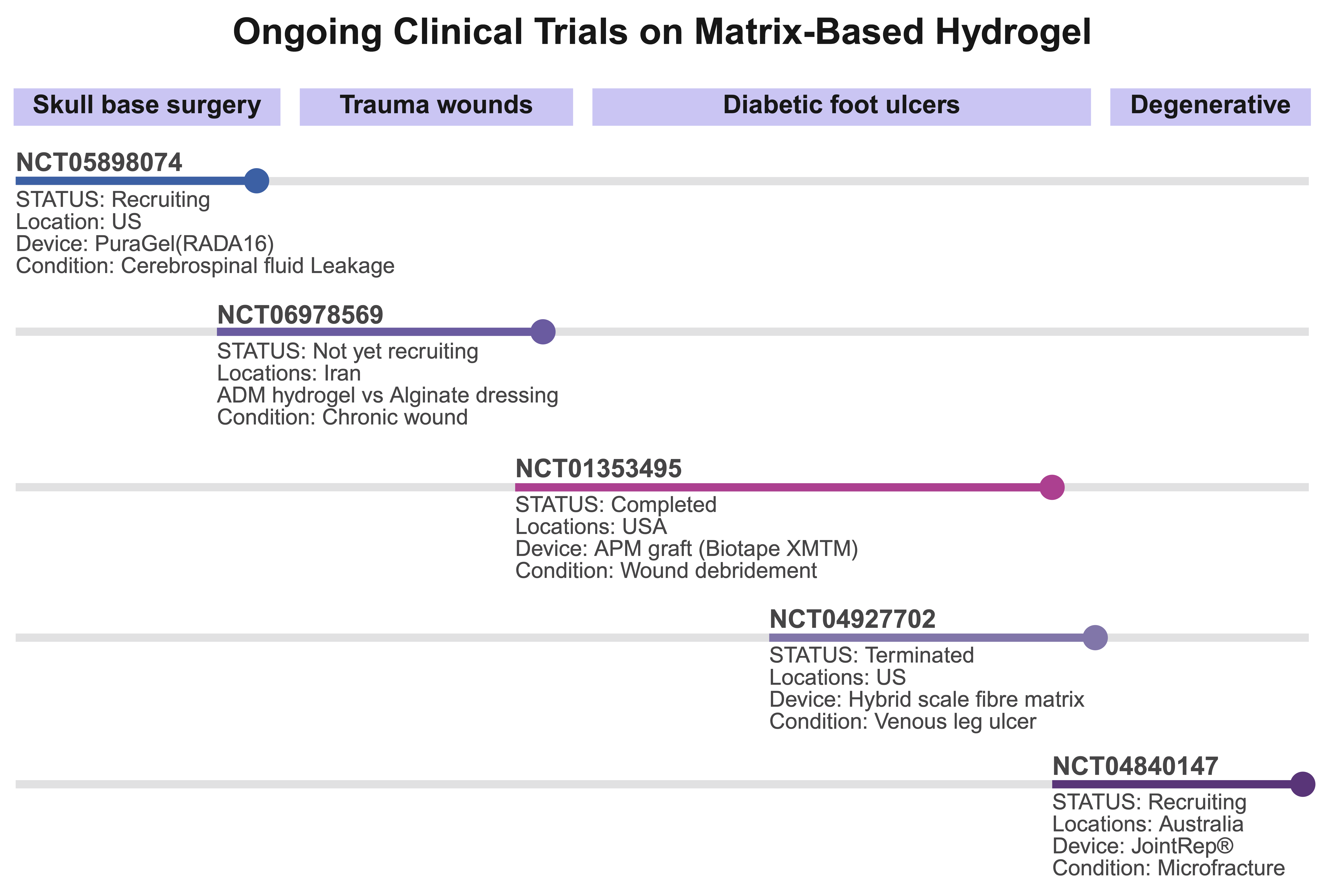
Ongoing clinical trials on matrix-based hydrogels across therapeutic areas. The timeline summarizes selected registered clinical studies investigating hydrogel applications in (i) skull base surgery (NCT05898074)
Intellectual-Property Trends (Patent Landscape 2020–2024)
The patent landscape for matrix-based hydrogels has expanded significantly over the past five years, reflecting the growing interest in both biomedical applications and translational potential 101. An analysis of patents filed between 2020 and 2024 revealed a focus on hydrogel design for tissue engineering, drug delivery, and organ-on-chip platforms. Key trends include innovations in crosslinking strategies, stimuli-responsive functionalities, and hybrid natural-synthetic formulations. Major stakeholders include academic institutions, biotech startups, and established medical device companies, highlighting both research-driven and commercially motivated development 102. This patent landscape provides insights into emerging directions, guiding future research and the potential commercialization of matrix-based hydrogel technologies.
Challenges and Emerging Solutions in Hydrogel Applications
Hydrogels hold immense potential for biomedical applications; however, translating laboratory innovations into clinical use requires addressing mechanical limitations, cost-effective production, scalability, and regulatory compliance issues. Regulatory considerations are critical for the successful clinical translation of hydrogel-based biomedical devices. Depending on device classification, the FDA may require either a 510(k) premarket notification or a more rigorous premarket approval (PMA) process. Sterilization compatibility is also essential, as standard methods such as γ-irradiation and ethylene oxide (ETO) can alter the hydrogel structure and functionality, necessitating careful optimization to preserve its mechanical and drug-release properties. Rather than viewing these as insurmountable barriers, ongoing research provides evidence-based solutions that are reshaping the field 103. A significant limitation of hydrogels, particularly in load-bearing applications (bone, cartilage, and skin), is their low mechanical strength and susceptibility to enzymatic degradation under physiological stress 104,105. Recent advances have demonstrated that incorporating nanocellulose, graphene oxide, or silica nanoparticles into nanocomposite matrices markedly enhances their tensile strength and elasticity, while maintaining cytocompatibility 106. For instance, Feng et al.107 reported a GO-GO-chitosan hybrid hydrogel with 4-fold higher compressive modulus than unreinforced gels, whereas Zhao et al. achieved similar mechanical gains using nanocellulose crosslinkers 108. The apparent variability stems from differences in crosslinking chemistry (hydrogen bonding vs. covalent grafting) and nanoparticle surface functionalization, which govern the load transfer and water retention. There is a consensus that dual-network and hybrid crosslinking (physical + covalent) approaches best balance the injectability, resilience, and degradation rate. However, contradictions remain regarding nanoparticle cytotoxic thresholds and long-term inflammatory responses, especially in cartilage or bone implantation models.
The reliance on specialized synthetic polymers and reactive crosslinkers often inflates production costs and complicates GMP compliance 109. Comparative studies have shown that bio-based hydrogels made from chitosan, alginate, or bacterial cellulose can achieve mechanical and biological properties comparable to those of PEG or PVA systems when processed via enzymatic crosslinking (e.g., transglutaminase or horseradish peroxidase). Enzymatic and radiation-induced crosslinking are now favored for their scalability and reduced chemical residue, supporting both environmental sustainability and regulatory acceptance. Industrial-scale manufacturing strategies, such as freeze–thaw cycling and radiation crosslinking, have been adapted to achieve batch consistency and sterility 110. The regulatory landscape is increasingly aligned with the ISO-10993 standards for biocompatibility, which govern cytotoxicity, genotoxicity, immunogenicity, and degradation byproducts. For instance, researchers developed a gelatin–hyaluronic acid–chondroitin sulfate hydrogel crosslinked using 1-Ethyl-3-(3-dimethylaminopropyl)-carbodiimide (EDC) and evaluated its safety according to ISO-10993-11 (acute systemic toxicity, implantation, and intracutaneous reactivity), demonstrating regulatory-grade preclinical validation 109. Early integration of ISO-compliant testing accelerates translational timelines and facilitates alignment with FDA and EMA GMP standards, particularly for drug-loaded and implantable systems 111. Despite promising preclinical outcomes, most pH-, enzyme-, and temperature-responsive smart hydrogels remain confined to early-stage trials. Emerging translational approaches couple multi-stimuli responsiveness with patient-specific molecular profiling, enabling personalized drug delivery and the development of regenerative strategies. However, reproducibility and response stability across patient cohorts remain key barriers. Comparing approved and experimental systems highlights the translational gap: ISO-compliant, clinically validated hydrogels (alginate wound dressings, hyaluronic acid fillers) exhibit consistent safety and mechanical predictability, whereas nanocomposite or smart hydrogels, although highly functional, face challenges in regulatory standardization and reproducibility (Table 4).
Commercially Approved Versus Experimental Hydrogel Systems in Biomedicine
| System | Application | Status | Key features/ Standards | Reference |
|---|---|---|---|---|
| Hyaluronic acid-based dermal fillers (Restylane, Juvederm) | Cosmetic/ soft tissue repair | FDA-approved | Injectable, ISO-10993 tested, well-established safety | |
| PEG-based hydrogels (TransCon, ReGel) | Sustained drug delivery (Oncogel) | Phase II trials | Thermosensitive, depot drug release GMP production | |
| Alginate wound dressings (Algisite, Kaltosite) | Wound healing | Commercially approved | Biopolymer-based, ISO-10993 compliant, hemostatic | |
| PNIPAAm-based thermoresponsive gels | Injectable scaffolds, drug delivery | Experimental | Preclinical, responsive to temperature, ISO testing limited | |
| Nanocomposite hydrogels (graphene oxide, nanocellulose reinforced) | Load bearing scaffolds cartilage repair | Preclinical | Enhance mechanical strength, regulatory evaluation pending | |
| Multi-stimuli responsive smart hydrogels | Targeted cancer therapy. biosensing | Preclinical /early trials | Precision-medicine oriented, reproducibility challenges |
A critical evaluation of different hydrogel classes reveals inherent trade-offs among mechanical strength, biodegradability, and biological performance, with natural polymers excelling in biocompatibility but lagging in durability 125. In contrast, synthetic polymers offer structural robustness at the expense of bioactivity (Table 5). Beyond materials science, emerging translational solutions include AI-guided hydrogel formulation optimization, organ-on-chip testing for preclinical biocompatibility, and in silico degradation modeling, which reduce animal use and accelerate approval. Collaboration among materials scientists, clinicians, and regulatory agencies is essential to standardize bench-to-bedside evaluation pipelines and ensure that hydrogel innovations achieve clinical and commercial viability 126.
Critical comparison of mechanical versus biological performance for the main hydrogel classes.
| Hydrogel Class | Mechanical Performance | Physical Performance | Advantages | Limitations | Reference |
|---|---|---|---|---|---|
| Natural hydrogels (Alginate, Chitosan, Collagen) | Generally low mechanical strength; limited load-bearing capacity; tunable by ionic/covalent crosslinking | Excellent biocompatibility and biodegradability; support for cell adhesion and ECM mimicry | Biodegradable, biocompatible widely available, natural ECM mimicry | Weak mechanics batch variability, faster degradation | |
| Synthetic hydrogels (PEG, PVA, PNIPAAm) | High reproducibility and tunable can be engineered for durability and stiffness | Limited bioactivity unless functionalized; low immunogenicity but poor cell adhesion | Reproducibility, controlled degradation, customizable properties | Lack inherent bioactivity may require modification, potential toxicity of crosslinkers | |
| Hybrid hydrogels (Natural and synthetic) | Improved strength compared to natural hydrogels; tailored stiffness via synthetic components | Balanced bioactivity; retain biocompatibility while offering structural reinforcement | Synergetic effect combines bioactivity of natural polymers with strength of synthetic | Complex fabrications, higher cost, reproducibility challenges | |
| Smart/stimuli-responsive hydrogels (pH, temperature, redox sensitivity) | Mechanical stability depends on the formulation; often softer but responsive | High potential in precision medicine can release drugs or signals in response to physiological triggers | Controlled and targeted drug delivery, responsive tissue engineering applications | Design complexity potential instability, limited large scale clinical translation so far |
Future Directions
The future of hydrogel research is poised for rapid expansion, with multiple exciting directions on the horizon. One promising avenue is the development of hydrogels that can respond to multiple stimuli simultaneously. Multi-responsive hydrogels, which can respond to combinations of physical, chemical, and biological cues, can provide sophisticated drug delivery systems that adapt to the dynamic environments within the body. For instance, such systems can release drugs in response to temperature and pH changes within a tumor, offering a dual-action approach to cancer treatment. Additionally, integrating biosensors into hydrogels could enable real-time monitoring of drug release and therapeutic efficacy, leading to personalized and adaptive treatments. The integration of bioinformatics and computational design methods is an exciting development. By applying advanced modelling techniques to predict the behavior of hydrogels in biological systems, researchers can optimize hydrogel design before synthesis, accelerating the development of new materials. Machine learning algorithms can also help identify novel polymer structures and fabrication techniques, thereby streamlining the discovery of hydrogels with specific functionalities. As our understanding of hydrogel behavior continues to improve, the potential to create fully autonomous hydrogel-based systems that dynamically respond to the body’s needs is increasing, thereby boosting the overall effectiveness of treatments. The future of hydrogel research is set for rapid growth, although many recent innovations remain preclinical or under regulatory review, with several exciting directions on the horizon that hold great promise.
Conclusion
Matrix-based hydrogels are a highly versatile and promising class of materials for drug delivery and other biomedical applications. Their ability to retain large amounts of water and provide a soft biocompatible matrix for the encapsulation of drugs, cells, or bioactive agents makes them ideal for a range of therapeutic applications. With advances in hydrogel synthesis and functionalization, hydrogels are now being developed to respond to specific environmental triggers, release drugs in a controlled and targeted manner, and adapt to patients changing needs. These innovations promise to revolutionize drug delivery, tissue engineering, wound healing, and other medical fields. Although significant progress has been made, the future of hydrogel technology in medicine depends on overcoming key challenges, such as improving mechanical strength, reducing production costs, and developing hydrogels that can respond more precisely to complex physiological signals. The ongoing development of multi-stimuli-responsive hydrogels, combined with the integration of bioinformatics and personalized medicine strategies, holds promise for these materials. As hydrogels continue to evolve, they are expected to play a central role in advancing therapeutic strategies and improving patient care. Hydrogels are a versatile and rapidly evolving class of biomaterials with significant potential for supporting next-generation therapeutic and diagnostic platforms. Taken together, the literature shows that hydrogel performance arises from interactions between polymer chemistry, network architecture, and additive components (nanoparticles, peptides, and drugs) rather than any single material property. Dual- or multi-stimuli systems outperform single-stimuli systems only when the stimuli operate through complementary, non-redundant mechanisms and when network reversibility and degradation kinetics are harmonized with the intended dosing regimen. Similarly, nanoparticle incorporation enhances functionality but requires careful optimization of size, surface chemistry, and loading to avoid undesirable immunogenicity or cytotoxicity. Therefore, moving hydrogel platforms from bench to bedside requires systematic cross-study comparisons, standardized characterization protocols, and long-term in vivo safety data.
Abbreviations
3D: Three-dimensional; ADM: Acellular Dermal Matrix; AI: Artificial Intelligence; Ca²⁺: Calcium ions; CDx: Companion Diagnostic; CFR: Code of Federal Regulations; CRISPR: Clustered Regularly Interspaced Short Palindromic Repeats; DNA: Deoxyribonucleic acid; ECM: Extracellular Matrix; EDC: 1-Ethyl-3-(3-dimethylaminopropyl)-carbodiimide; EMA: European Medicines Agency; ETO: Ethylene Oxide; FDA: Food and Drug Administration; GMP: Good Manufacturing Practice; GO: Graphene Oxide; HA: Hyaluronic Acid; IPN: Interpenetrating Polymer Network; ISO: International Organization for Standardization; MDR: Multidrug-resistant; mRNA: Messenger Ribonucleic Acid; PEG: Poly(ethylene glycol); PMA: Premarket Approval; PNIPAAm: Poly(N-isopropylacrylamide); PVA: Poly(vinyl alcohol); RADA16: Arginine-Alanine-Aspartic Acid-Alanine 16-mer peptide; RGD: Arginylglycylaspartic acid; RNA: Ribonucleic acid; UV: Ultraviolet; WOS: Web of Science
Acknowledgments
We thank BioRender for providing a platform that improved the graphical representation. Figures 1, 3, 4, and 5 were created using BioRender (https://app.biorender.com/) with permission to publish.
Author’s contributions
RS and RSh conceptualized the study. AR, RS, and RSh conducted analyses, drafted, and revised the manuscript. DS, RB, and AC analyzed and reviewed the manuscript.
Funding
None.
Availability of data and materials
Data and materials used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Declaration of generative AI and AI-assisted technologies in the writing process
The authors declare that they have not used generative AI (a type of artificial intelligence technology that can produce various types of content including text, imagery, audio and synthetic data.
Competing interests
The authors declare that they have no competing interests.

